My Story:
Timothy
From Christchurch
Timothy was born in Christchurch on 19 October 2022. He’s our precious boy, a little brother to Thomas, and a joy to Fen and me. As we share Timothy’s journey, he is currently facing a second relapse of hepatoblastoma.
At this stage, the New Zealand medical system has no more treatment options for him, so we are still actively looking for help from hospitals in other countries.
Compared to when we first heard the diagnosis, we’ve learned to face this reality with a much calmer heart. We are so truly grateful to everyone who has cared for us and walked with us along the way. You have brought a deep, lasting comfort to our hearts that we can’t even put into words.
1. The Diagnosis of Hepatoblastoma
The story began on 20 July 2023. It all started on 20 July 2023. Fen took Timothy to see Plunket, and the nurse noticed his tummy was really swollen and felt quite hard. She told us to see a GP as soon as possible. We saw the GP on July 23, and they realised right away there was something serious with Timothy’s liver and sent us straight to the Emergency Department at Christchurch Hospital.
Then came all the intensive tests. As parents going through this for the first time, we were shocked, scared, and felt completely lost. We kept praying and hoping it wouldn't be anything too bad. But the doctors told us it was most likely a form of liver cancer. They arranged a CT scan, MRI, and biopsy to confirm everything, and we were moved to the oncology team. Those days felt like they would never end. We cried so much, asking "Why is this happening?" Watching Timothy go through all that pain and those tests made us feel so guilty—we wished so much we could just take his place. Our friends and church gave us so much help and comfort, but we realised then that we needed time to process everything and find a deeper kind of peace.
2. The Start of the First Chemotherapy
After the biopsy was done on 28 July 2023, Fen noticed Timothy was starting to swell up all over his body. We told the medical team immediately. An ultrasound showed the tumour was pressing on a nearby vein, blocking his circulation. The doctors told us Timothy’s life was in danger if he didn’t start treatment right away. So, we started chemotherapy on the night of July 30.
Once the chemo started, the oncology team confirmed the results: it was definitely Hepatoblastoma. Because the tumour was so massive, the plan was to do 2–3 rounds of chemo first, followed by a mandatory liver transplant. That transplant could only be done at Starship Hospital in Auckland.
3. Travelling to Auckland:
Preparing for the Liver Transplant On 21 August 2023, we travelled to Starship in Auckland for the first time. From Monday to Wednesday, we met the liver transplant and surgical teams. They went into a lot of detail about the surgery, the risks, and what life would be like after. We went back to Christchurch for more chemo and Timothy was put on the waiting list. Since New Zealand is so small, finding a donor liver is really hard. On August 30, I went through a donor assessment in Auckland, hoping I could be a living donor. But because of how my blood vessels are shaped, I didn't pass the assessment.
4. A Decision While Waiting:
Living Donor Transplant After Timothy's third round of chemo, the team in Auckland decided to pause treatment for two weeks to see if a deceased donor liver would come up. Since we had to be there the moment a liver was available, we decided to move the whole family to Auckland early on September 9 to wait. At the same time, Fen told the doctors she was willing to be a living donor, so they started her assessment.
5. The First Surgery: Liver Transplant (22 September 2023)
From 11 to 14 September 2023, Fen went through all the tests—16 tubes of blood, urine tests, scans, the lot. It turned out her liver was very healthy and she was a perfect match. The doctors decided that if no other liver came up, Fen would donate part of hers to Timothy on the morning of 22 September at 7:00 am.
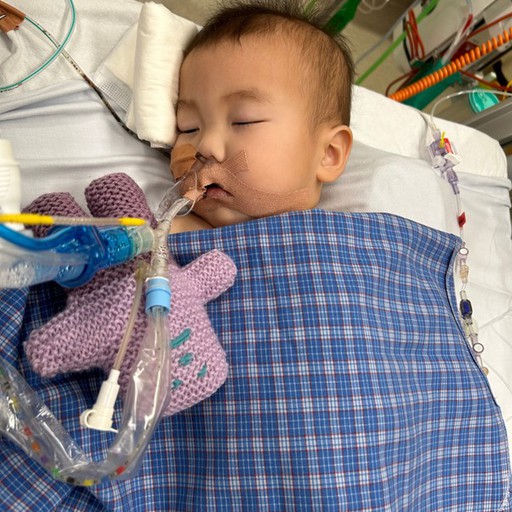
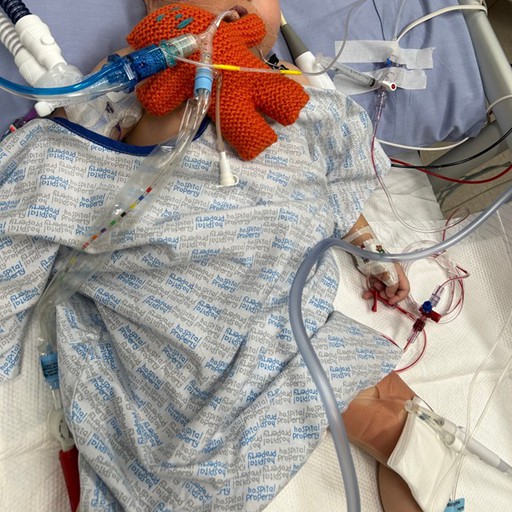
That was such an incredibly long day. Fen went in for surgery just after 6:00 am, and Timothy followed soon after. Her surgery took about five hours, and Timothy’s took eight. When Fen was back in the ICU, Timothy was still in theatre—he didn't finish until 8:00 pm. I finally saw him in the PICU at 10:00 pm. Seeing him covered in all those tubes and wires was heartbreaking, but we were so thankful to God that both surgeries were a success. That day, Timothy was only 11 months old, and he had already been through so much.
6. Recovery and Further Chemotherapy
After the surgery, they both did quite well overall. But because Timothy needed his mum so much, Fen only rested in the ward for 4 days before she started taking care of him—even before she had fully recovered herself. It was such a hard time. Fen pushed through her own pain to stay by Timothy’s side, breastfeeding and comforting him.
Two weeks later, Timothy was discharged and our family moved into the Ronald McDonald House together. During his hospital stay, he had one episode of moderate liver rejection and needed blood tests every day. From 12 October, he finished his fourth and fifth rounds of chemo at Starship. On 5 November, after eight weeks in Auckland, we finally got to go home to Christchurch.
7. The Second Surgery:
Intestinal Perforation and Lymphoma Diagnosis After the transplant, Timothy’s kidney function never fully recovered. After talking to a medical team in the US, the doctors decided to cancel his sixth round of chemo. He was having blood tests all the time because he had to take the anti-rejection med Tacrolimus (tac). He wasn't sleeping or eating well, and he wasn't gaining much weight, which really worried us. From December 2023, his levels became really unstable. In February 2024, things got worse—he had high potassium, anaemia, CMV infection, and constant fevers. We were in and out of the hospital constantly. Sometimes we’d see Timothy just lying flat on the floor in pain, but no one knew why. On 7 March 2024, Timothy was brought back to the ER for persistent abdominal pain. The doctors thought it was cholangitis and gave him a five-day course of antibiotics.
This caused severe diarrhoea and really loud stomach sounds. Seeing his liver function return to normal, they discharged him. But after returning home, he didn't truly improve. On the evening of Easter Holiday-1st of April, we took him back to the ER. The doctors again suspected cholangitis and gave him two more weeks of antibiotics. On 5 April, they did a biopsy thinking it might be liver rejection, but 1 week later the liver turned out fine. By the end of those two weeks, the antibiotics had just made his diarrhoea and stomach pain worse. His tac levels stayed high even though his dose was very low. On 16 April, with no clear answer of the tummy pain, he was discharged. That night at 10:00 pm, things went wrong very fast. His face turned pale and grey, and he started moaning and vomiting. We rushed him to the ER. He was in shock and in so much pain that even morphine didn't work.
Timothy was in agony all night, begging us for water. Because he couldn't lie down, Fen held him in a chair the whole night while he just moaned with his eyes open. Later, when we learned about intestinal perforation (a hole in the bowel), we realised how much pain he must have been in. On 17 April, scans showed a large amount of fluid in his abdomen. The surgical head examined him and ordered an urgent CT scan, which revealed a hole in his intestine and his diaphragm. He needed surgery within 30 minutes or he wouldn't make it. After enduring 24 hours of pain, Timothy underwent his second operation. Facing this crisis again was another huge challenge for us.
8. The Lymphoma Diagnosis and Treatment
During the surgery, they removed about 5cm of his small intestine. Because they were worried about a potential chest infection, they didn't fix the hole in his diaphragm during that operation. Timothy’s condition improved a lot after the surgery, but while he was in the ICU, the biopsy results came back: the hole was caused by the EBV virus, which had triggered cancerous changes in the lymph tissue around it. He was diagnosed with lymphoma. Because the doctors suspected it was PTLD (PostTransplant Lymphoproliferative Disorder), Starship arranged for Timothy to be transferred by air ambulance back to Auckland for more tests and treatment. After the medical team at Starship discussed everything, they decided on a treatment plan: Rituximab combined with Cyclophosphamide, for a total of six cycles of chemotherapy, once every three weeks.
9. The Third Surgery: Bowel Obstruction and Diaphragm Repair
We stayed in Auckland for about four weeks. Once Timothy’s condition was stable, we returned home to Christchurch on 21 May 2024, where he continued his treatment with Rituximab and Cyclophosphamide at Christchurch Hospital. After the surgery for his bowel perforation, the doctors changed his anti-rejection medicine from Tacrolimus to steroids because tac is not suitable for him. As the Rituximab and other meds were so hard on his immune system, his immune markers stayed very low all the time. As a result, whenever he wasn't in the hospital for chemo, we were constantly back in the emergency department with fevers and other complications.
On 17 July, Timothy was discharged after his fourth round of chemo. But within just two days, he was back in the hospital with a fever and other symptoms, and he wasn't discharged again until 27 July. That very same evening, Timothy started having abdominal pain, he couldn't pee, he was very lethargic, and he started vomiting—so we found ourselves rushing back to the hospital once again. He was so unwell. He couldn't keep any food down, he was desperately thirsty, and the pain in his tummy just kept getting worse. Paracetamol did nothing, and even morphine couldn't settle him down. The pain this time was just as bad as when his bowel burst before, and it lasted for about 24 hours. The medical team did an ultrasound, X-ray, and CT scan. The ultrasound looked normal. But the X-ray showed that more of his intestine had moved up into his chest, crushing his right lung and making it very hard for him to breathe and causing terrible pain. The CT scan confirmed it was a bowel obstruction, and he needed surgery right away.
The biggest worry was that without surgery, the bowel could die (become necrotic). If that happened and they had to remove part of his large intestine, Timothy would have needed a stoma bag on his tummy until his bowel could work again— that was a thought that really terrified us. Timothy’s surgery was finally finished at 3:30 in the morning on 29 July. Thank God, his large intestine was okay. The surgery went well—the surgical team put the bowel back where it belonged and repaired the hole in his diaphragm. By this point, Timothy’s tummy had been opened up three times in the exact same spot.
10. The Fourth Surgery:
Lung Nodule Removal and Hepatoblastoma Relapse During the CT scan before his diaphragmatic hernia fix surgery, the doctors accidentally found two spots on Timothy’s left lung. Since his tumour markers (AFP) had been going up for two months, the team was worried the cancer was back and decided to remove the nodules for a biopsy as soon as possible. On 7 August 2024(Just one week after the previous surgery), Timothy had surgery again to remove the spots from his left lung.
On 19 August, it was confirmed: the hepatoblastoma had relapsed and spread to his lungs. This meant he had to start even stronger chemo—six cycles in total, once every three weeks. Because the drugs were so powerful, Timothy’s immune system stayed at a near-zero level the whole time. The side effects were awful every single cycle: constant vomiting, diarrhoea, high fevers, and feeling extremely ill. He had no appetite at all and couldn't even manage feeding through a tube, so he lost weight very fast. After talking with the medical team, he was put on TPN (feeding through a vein) to help him gain weight between cycles so his body could handle the next round.
During those six months, we were basically always in the hospital or on our way there. It was exhausting. To make it even harder, Timothy carried the ESBL (ExtendedSpectrum Beta-Lactamase) bacteria from Starship , which meant he had to stay inside his hospital room at all times. As he grew and wanted to do more, he would cry out loudly whenever he was unhappy or uncomfortable, and it was so hard to calm him down. It made a difficult time even harder for everyone. We finally finished that round of chemo in December 2024.
11. The Second Recurrence of Hepatoblastoma
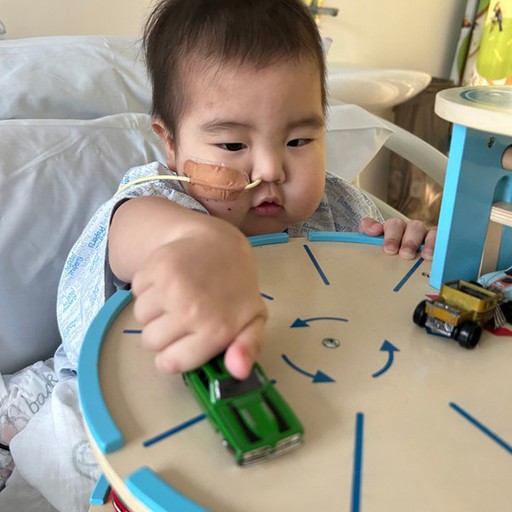
It took about three months after chemo for Timothy to start feeling like himself again. He still wasn't sleeping well, but in other ways, he was doing so much better— smiling, laughing, and running around with so much energy every day. But we noticed his development was slower than other kids his age. Fen had mentioned to the doctors that he wasn't speaking much, didn't really play with other children, and was very sensitive to touch. In May 2025, a psychologist assessed him and found that Timothy has autism. We don't know if it was from the treatment or something he was born with, but the hospital helped us find support, and we eventually chose the Champion Centre.
We saw Timothy getting stronger every day and truly thought we were moving in the right direction. But in June 2025, his AFP levels started rising again. On 5 July, the oncologist told us the cancer was likely back for a second time, and New Zealand had no more treatment options left for him. He was moved to palliative care, and a nurse was assigned to help our family. But seeing Timothy so happy and full of life, we felt we had to keep looking for a way. We asked for second opinions from Starship and talked to hospitals in Canada and China. We eventually decided to try a cancer medication, though we aren't sure yet if it will work. Timothy still runs around happily every day, goes to kindergarten, and attends the Champion Centre. A pharmacist even made a special melatonin for him that he can tolerate, which has finally helped him sleep. We don't know what the future holds, and we know he might leave us suddenly one day, but we are at peace with that.
What a courageous family, having gone through so much. Praying for a cure for Timothy in 2026. Thankyou for sharing your story. It will surely help other families facing similar challenges. Wishing you all the best for the future. IDFNZ
Words of Gratitude
Looking back, this isn’t just Timothy’s
story—it’s the story of how God has grown
our whole family.
We started this journey in total shock,
feeling so helpless. Like any parents, we
tried so hard to control every outcome and
fix everything ourselves. But through all
the hospital stays and the surgeries, we’ve
slowly learned to let go. We’ve realised
that our lives, and Timothy’s life, aren't in
our hands—they are in His.
Timothy at the preschool
We have now been able to hand Timothy
over completely into God’s care. That
has been our real journey of growth.
We’ve learned that even though we can't
always avoid these hard trials, we can
support each other through love and
companionship.
We feel so blessed to live in New Zealand.
We are so thankful to the Government
for the free healthcare, which let us focus
entirely on being there for Timothy. A
huge thank you to the medical teams in
Christchurch and at Starship for their heart,
their patience, and for always listening
to us. And to IDFNZ, the Child Cancer
Foundation, Ronald McDonald House, and
so many others—thank you for walking
with us. A special thanks to IDFNZ for
making sure we had food that felt like
home while we were in Auckland.
We are still on the journey — and we
remain full of gratitude.